Table of Contents
The U.S. Department of Health and Human Services declared a public health emergency due to the increasing rates of opioid misuse, addiction, overdoses, and deaths.
The increasing number of opioid prescription medications that were prescribed starting in the late 1990s has led to widespread misuse of both illicit and prescription opioids.
If you or someone you love is addicted to opioids, it’s important to know how to recognize the signs of overdose and understand the basics of overdose prevention.
Acting quickly and in the correct manner can save someone’s life if they are overdosing. Let’s take a look at what you need to know about opioids and overdose prevention.
Opioid Overdose: The Basics
In 2019, opioids were involved in more than 70% of all of the drug overdose deaths that occurred. Out of the more than 70,000 drug overdose deaths in the US during that year, nearly 50,000 of them involved the use of opioids.
This means that opioids are currently the main driver of opioid deaths in the United States. Synthetic opioids other than methadone are particularly responsible.
All opioids, including prescription pain relievers, heroin, and synthetic opioids can lead to misuse and addiction. The number of people who are addicted and the number of overdoses and deaths amount to a serious national crisis that impacts public health in addition to economic and social well-being.
The opioid crisis has its roots in the late 1990s when pharmaceutical companies reassured the community of medical professionals that the use of prescription opioid pain relievers would not lead to addiction. During this time, they began to be prescribed at a greater rate. This then lead to these medications becoming widely diverted and misused.
On top of that, the rise of drugs being laced with illicitly manufactured fentanyl also increased the number of overdoses and deaths attributed to opioids.
Sometimes it can be difficult to know whether or not you are suffering from an addiction. Take our online test today to help you understand whether you have a problem with drugs or alcohol.
The Different Types of Opioids
Opioids are a class of drugs that include both opiates and synthetic opioids. Opiates are drugs that are derived from the opium poppy, while synthetic opioids are synthesized in a lab and act on the same areas of the brain as opiates do.
Examples of opiates:
- Heroin
- Morphine
- Opium
- Codeine
Examples of synthetic opioids:
- Oxycodone
- Methadone
- Hydrocodone
- Fentanyl
There are a number of different opioids that are prescribed as pain-relievers. These include morphine, oxycodone, hydromorphone, and hydrocodone.
Opioids work by attaching themselves to opioid receptors in the brain and body. They exert their effect wherever they attach to these receptors. Our body actually produces opioids but never in amounts that could lead to an overdose.
Opioids can reduce pain by affecting the spinal cord, acts on the limbic system to create feelings of relaxation and pleasure, and can slow breathing and heartbeat.
The Rise of Fentanyl Laced Heroin
Fentanyl is a type of synthetic opioid. It is produced pharmaceutically and prescribed for the treatment of severe pain, such as that experienced by advanced cancer patients. This drug is 50 to 100 times more potent than morphine.
Prescription fentanyl can be and has been diverted for both misuse and abuse. On top of that, fentanyl is also illicitly produced and sold through illegal drug markets.
It is also sometimes mixed with drugs such as heroin and cocaine in order to increase the euphoric effects of drugs. Users of these drugs may or may not be aware of the fact that the drugs they are using contain fentanyl.
Between 2018 and 2019, the rates of overdose deaths that involved synthetic opioids (other than methadone) rose by 16%. In 2019 alone, more than 36,000 people died in the United States from overdoses that involved synthetic opioids. It is anticipated that the number of overdose deaths has accelerated as a result of the coronavirus pandemic and its fallout.
The Drug Enforcement Agency recently made its first public safety announcement in six years warning about a significant increase in fake prescription drugs available on the black market that contains fentanyl at potentially lethal doses. These pills are made to look like legitimate prescription medications and are sold online and on the street.
Overdose Prevention: What You Need to Know
According to the CDC, the most effective forms of opioid overdose prevention are reducing exposure to opioids, improving opioid prescribing, treating opioid use disorder, and preventing misuse.
It can be difficult to recognize an opioid overdose. If it isn’t clear whether or not someone is overdosing, the CDC recommends treating the situation as if it is an overdose. This means that you should seek medical care or call 911 and make sure that the person is not left alone.
Some of the signs of an overdose might include:
- Slow, shallow breathing
- Limp body
- Choking or gurgling sounds
- Loss of consciousness or falling asleep
- Constricted, small "pinpoint pupils"
- Blue, cold, or pale skin
People who use opioids are at a higher risk of overdose during certain situations. For example, mixing opioids with alcohol, anxiety pills, or sleeping pills increases the risk of overdose. This is also true if an individual mixes opioids with other opioids or a number of different prescription medications.
Using opioids in an unfamiliar setting or alone can also increase the likelihood of overdose as well as starting to use opioids again after a period of not using or cutting down. The risk of overdose increases when a person uses a new supply or increases their opioid dose.
Understanding Naloxone
Naloxone is a medication that can reverse an opioid overdose rapidly. It is able to reverse and block the effects of other opioids by attaching to opioid receptors. The term for this type of drug is an opioid antagonist.
This is not a treatment for opioid use disorder. However, if a person’s breathing has stopped or slowed due to an overdose on opioids, naloxone can restore normal breathing quickly.
When a person is showing signs of an overdose, naloxone can be given as an injection or as a nasal spray.
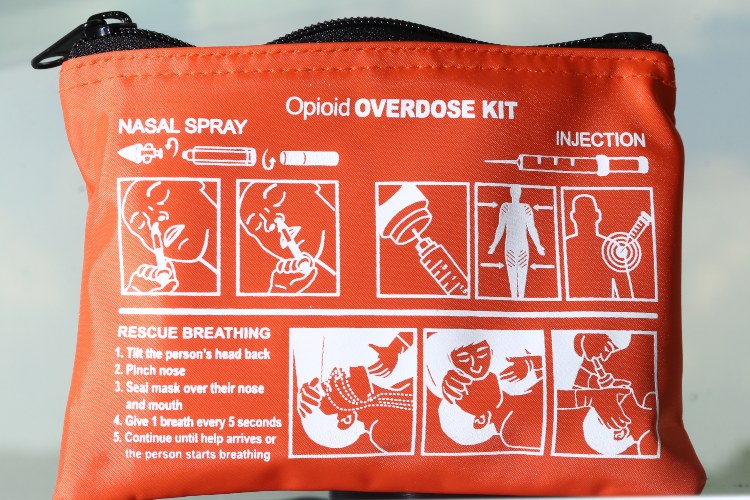
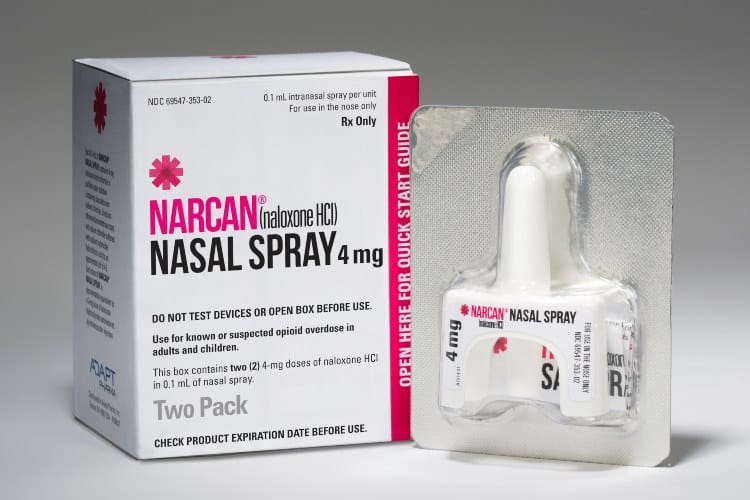
How to Get Naloxone
Naloxone may be available for purchase at your local pharmacy. In many states, you can get Naloxone as well as training on how to use Naloxone free of charge. Policies vary depending on the pharmacy you visit and where you live. But here is a shortlist of large pharmacy chains that provide Naloxone without the need for a prescription.
- CVS: Naloxone is available without a prescription at most CVS pharmacies.
- Walmart & Sam’s Club: Walmart and Sam’s Club will dispense naloxone without a prescription in all states where state law allows them to.
- Kroger: Naloxone is available without a prescription in all Kroger stores.
- Walgreens: Naloxone is available without a prescription in over 8,000 locations.
- Rite Aid: Rite Aid offers naloxone without a prescription at all of its pharmacies in 19 states.
Call your pharmacist to see if you can still get naloxone without a prescription at a location near you. You can also go to the Naloxone finder website to see resources in your area. This video from the National Institute on Drug Abuse explains the initiative to make Naloxone more readily available to the public.
Responding to an Opioid Overdose
If there is someone experiencing a medical emergency, the first thing you should do is call 911 right away. Acting quickly is absolutely essential in this scenario.
It typically takes somewhere between a few minutes and a few hours for a person to die from an overdose. When people survive opioid overdoses, it is because there was another person there that responded.
If a person is overdosing on opioids, they will be not responsive and not breathing.
1. Yell the person’s name and administer a hard sternum rub to their chest plate
• Call the person’s name.
• If this doesn’t work, vigorously grind knuckles into the sternum (the breastbone in middle of chest) or rub knuckles on the person’s upper lip.
• If the person responds, assess whether he or she can maintain responsiveness and breathing.
• Continue to monitor the person, including breathing and alertness, and try to keep the person awake and alert.
2. Use naloxone/Narcan if you have it, administering one dose every two minutes
If the person overdosing does not respond within 2 to 3 minutes after administering a dose of naloxone, administer a second dose of naloxone. Naloxone should be administered to anyone who presents with signs of opioid overdose or when opioid overdose is suspected. Naloxone is approved by the Food and Drug Administration (FDA) and has been used for decades by EMS personnel to reverse opioid overdose and resuscitate individuals who have overdosed on opioids.
Research has shown that women, older people, and those without obvious signs of opioid use disorder are under-treated with naloxone and, as a result, have a higher death rate. Therefore, it is also important to consider naloxone administration in women and the elderly found unresponsive with opioid overdose. Naloxone can be given by intranasal spray and by intramuscular (into the muscle), subcutaneous (under the skin), or intravenous injection.
All naloxone products are effective in reversing opioid overdose, including fentanyl-involved opioid overdoses, although overdoses involving potent (e.g., fentanyl) or large quantities of opioids may require more doses of naloxone.
3. Call 911 and tell them that an individual is not breathing and not responsive
An essential step is to get someone with medical expertise to see the person as soon as possible. If no emergency medical services (EMS) or other trained personnel is on the scene, activate the 911 emergency system immediately. All you have to say is “Someone is unresponsive and not breathing.”
Be sure to give a specific address and a description of your location. After calling 911, follow the dispatcher’s instructions. If appropriate, the 911 operator will instruct you to begin CPR (technique based on rescuer’s level of training
4. Provide rescue breathing
Ventilatory support is an important intervention and may be lifesaving on its own. Rescue breathing can be very effective in supporting respiration, and chest compressions can provide ventilatory support. Rescue breathing for adults involves the following steps:
• Be sure the person’s airway is clear (check that nothing inside the person’s mouth or throat is blocking the airway).
• Place one hand on the person’s chin, tilt the head back, and pinch the nose closed.
• Place your mouth over the person’s mouth to make a seal and give two slow breaths.
• Watch for the person’s chest (but not the stomach) to rise.
• Follow up with one breath every 5 seconds.
Chest compressions for adults involve the following steps:
• Place the person on his or her back.
• Press hard and fast on the center of the chest.
• Keep your arms extended
5. Roll the person on their side when they start to breathe on their own regularly
All people should be monitored for recurrence of signs and symptoms of opioid toxicity for at least 4 hours from the last dose of naloxone or discontinuation of the naloxone infusion. People who have overdosed on long-acting opioids should have more prolonged monitoring. Most people respond by returning to spontaneous breathing. The response generally occurs within 2 to 3 minutes of naloxone administration. (Continue resuscitation while waiting for the naloxone to take effect.)
Because naloxone has a relatively short duration of effect, overdose symptoms may return. Therefore, it is essential to get the person to an emergency department or other source of medical care as quickly as possible, even if the person revives after the initial dose of naloxone and seems to feel better.
If a person isn’t able to talk or walk well after they have woken up, it’s essential that they go to the hospital. Stay with the individual for several hours if possible and ensure that they stay awake.
Attending a rehab program can be necessary when someone is suffering from an addiction to powerful drugs such as opioids. If you’re looking for a rehab center in San Diego, check out this article to learn about your options.
Is It Time For You to Get Your Life Back?
Understanding overdose prevention is essential if either you or someone you love struggles with opioid addiction.
Facing an opioid addiction can be one of the most difficult issues that any person could ever face. Opioid use disorder can completely consume your life and puts you at risk of overdose and death.
If you’re addicted to any kind of opioid, there is help for you. At our San Diego rehab centers, our addiction specialists and case managers are highly trained in evidence-based methods of recovery. As a part of our program, you will be treated with tested and proven methods to both treat withdrawal symptoms and teach techniques for relapse prevention.

Medically Reviewed By:
Dr. Sanjai Thankachen
Dr. Sanjai Thankachen graduated from Adichunchanagiri Institute of Medicine in 2000. He completed his residency in psychiatry in 2008 at Creedmoor Psychiatric Center in New York. Dr. Thankachen is currently working with Pacific Neuropsychiatric Specialists in an outpatient practice, as well as working at multiple in-patient psychiatric and medical units bringing his patients the most advanced healthcare treatment in psychiatry. Dr. Thankachen sees patients with an array of disorders, including depression, bipolar illness, schizophrenia, anxiety, and dementia-related problems.

Edited for Clinical Accuracy By:
Sean Leonard, Psychiatric Nurse Practitioner
Sean Leonard is a board-certified psychiatric nurse practitioner. He received his master’s degree in adult geriatric primary care nurse practitioner from Walden University and a second postmaster specialty in psychiatry mental health nurse practitioner from Rocky Mountain University. Sean has experience working in various diverse settings, including an outpatient clinic, inpatient detox and rehab, psychiatric emergency, and dual diagnosis programs. His specialty areas include substance abuse, depression, anxiety, mood disorders, PTSD, ADHD, and OCD.
Sources
Assistant Secretary of Public Affairs (ASPA). (2021, February 19). About the Epidemic. HHS.Gov. https://www.hhs.gov/opioids/about-the-epidemic/index.html
Drug Overdose Deaths | Drug Overdose | CDC Injury Center. (2021, October 25). Centers for Disease Control and Prevention. Retrieved October 25, 2021, from https://www.cdc.gov/drugoverdose/deaths/index.html
The DEA Is Warning Of A Rise In Overdose Deaths From Fake Drugs Laced With Fentanyl: NPR. (2021, September 27). National Public Radio. https://www.npr.org/2021/09/27/1040899776/dea-public-safety-alert-fake-prescription-drugs-fentanyl?t=1635178919627
Get Naloxone Now. (2021, October 25). Get Naloxone Now. https://www.getnaloxonenow.org/

